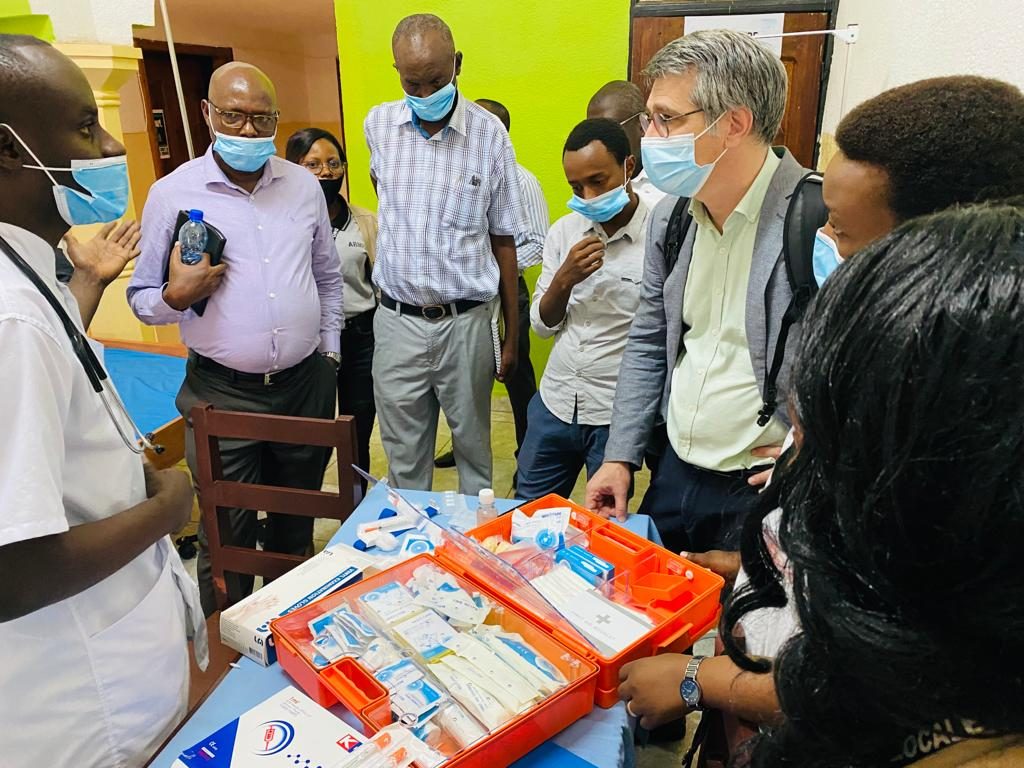
One year after the Nyumviriza project began, VHA, with other partners, received expertise France at Nyumviriza Centre, which funded the three-year project. The team led by Pauline experienced how activities are carried out in the Nyumviriza centre, where the VHA medical centre is. They are satisfied with the VHA medical team’s progress in treating people who use drugs.
The VHA’s dedicated team continues to provide harm-reduction services to drug users through medical consultations, disease diagnosis, and free medical treatment with medicines.
We are also excited to announce that rapid urine tests to determine the type of drugs taken are now available at our centre.
This is the next step in introducing opioid agonist therapy (methadone) for drug users in the future.
 The VHA will continue working with its partners to advocate for better harm reduction policies, programs, and practices to reduce drug use’s adverse health, social, and legal consequences.
The VHA will continue working with its partners to advocate for better harm reduction policies, programs, and practices to reduce drug use’s adverse health, social, and legal consequences.
In its daily operations, the VHA adheres to the harm reduction philosophy based on justice and human rights. The team focuses on positive change and works with drug users without passing judgment, coercion, discrimination, or requiring people to stop using drugs as a condition of receiving assistance.



 The project aims to contribute to developing a community-based harm reduction response, i.e. empowerment and capacity building through active participation of drug users. Drug users were encouraged to define the necessary health responses and ways to combat the stigma and exclusion of which they are victims. As a result, they are project actors who participate in planning, implementation, and evaluation phases.
The project aims to contribute to developing a community-based harm reduction response, i.e. empowerment and capacity building through active participation of drug users. Drug users were encouraged to define the necessary health responses and ways to combat the stigma and exclusion of which they are victims. As a result, they are project actors who participate in planning, implementation, and evaluation phases.